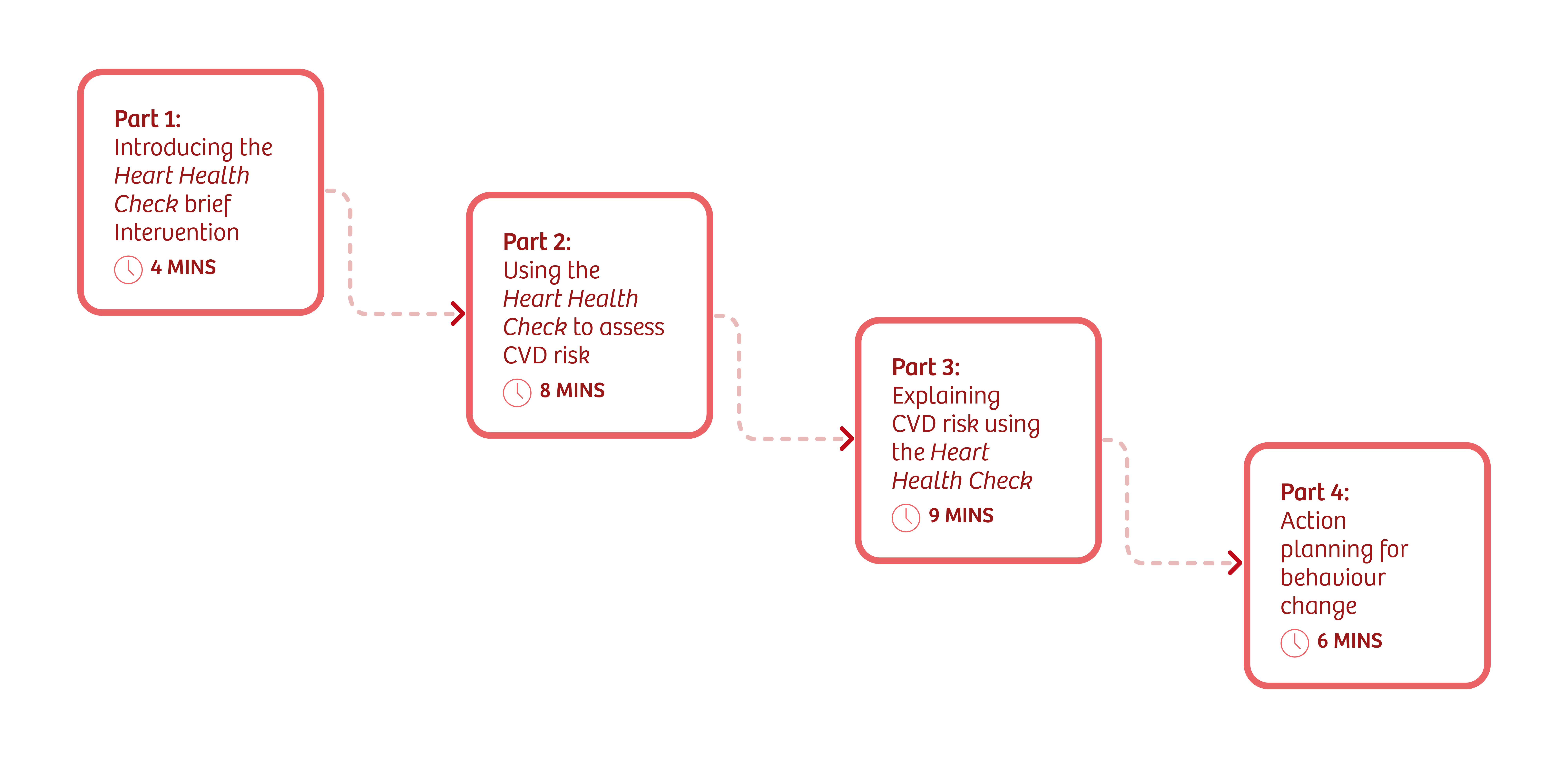
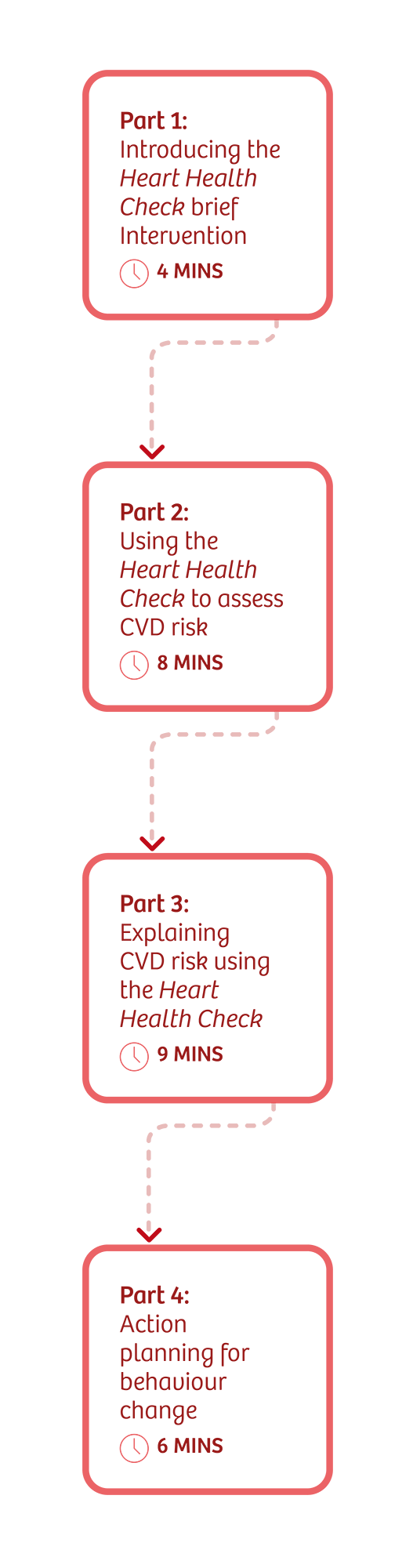
Introducing the Momenta Heart Health Check
What is the Heart Health Check?
The Heart Health Check is a tool designed to support patients with one or more risk factors for cardiovascular disease (CVD), aiming to stimulate them to change their behaviour to reduce their CVD risk. It’s based on research showing the success of similar brief interventions for smoking cessation, alcohol reduction and obesity management.
How is it delivered?
It’s available in two formats for use at in-person appointments or as an online tool for direct patient access. Both formats provide patients with personalised feedback and are free of charge to NHS staff.
1. In-person Heart Health Check
This paper-based tool has been designed flexibly to support a wide range of healthcare professionals with conversations in a variety of in-person appointments ranging from 5-20 minutes in length. For example:
- Following hypertension diagnosis
- In long-term condition or medication reviews
- After NHS Health Checks
In shorter appointments, patients can be signposted to complete some or all of the intervention themselves using the online tool (see below).
Resources include:
- Two-sided A4 printable document to help guide discussion
- Four short online training videos (less than 30 mins in total) explaining the intervention and giving examples of how it can fit into care pathway

Implementing the in-person tool
This is a simple three-step process:
- Download and print the two-sided A4 resource which helps to guide and support the conversation with the patient
- Identify who will deliver the intervention
- Ask them to complete the online training – four short videos totalling less than 30 minutes.
You can find out more about the in-person brief intervention and training for healthcare professionals by watching this short video, which is the first training module.
2. Online Heart Health Check
Where appointment time is short or unavailable, patients can access a standalone web-based version of the Heart Health Check to complete themselves. It guides them through a series of short questions related to their CVD risk factors and lifestyle. On completion, they receive an online personalised report based on their responses. This supports them to identify and plan changes to relevant lifestyle behaviours to improve their heart health, e.g. smoking, alcohol, physical activity and nutrition.
How can it be made available to patients?
In shorter appointments, healthcare professionals can complete the very first part of the tool with the patient which helps them to understand their risk factors e.g. high blood pressure then signpost them to complete the online Heart Health Check.
Alternatively, you can send link by text to a larger number of patients who might find the Heart Health Check helpful, e.g. after a register search. Experience indicates that uptake is likely to be higher if texts are signed off by a named individual, e.g. doctor or nurse rather than a generic practice communication.
Why has it been developed?
A number of tools are used to assess and highlight patients’ risk of developing CVD e.g. QRISK, heart age calculators etc. However, discussions with healthcare professionals (HCPs) highlighted the need for a simple, flexible tool and accompanying training to enable a wide range of HCPs to deliver a brief intervention using proven behaviour change approaches. The aim is to make the best use of the limited time available with patients, helping them move beyond a recognition of risk to identifying and planning realistic, relevant and achievable behaviour changes. Recognising the many pressures on resources and variety of possible uses the Heart Health Check needed to be flexible – and, ideally, free.
We are grateful to have secured NHS innovation funding to develop the Heart Health Check from SBRI and the Advanced Access Collaborative, and to our many project partners who have supported developing this resource, including the West Midlands Academic Health Science Network, NHS Birmingham and Solihull, the South Eastern Health and Social Care Trust and British Society of Lifestyle Medicine amongst many others.
On a separate but related note we are seeking funding to enable more people to access our CVD Prevention Programme, including for those who have used the Heart Health Check and are keen to embark on a supportive behaviour change programme. Please add your details here if you’d like to hear from us if we secure funding for the programme in your area.
We will not share your details with others or use them for any other purpose.
Register interest
What is Momenta?
Momenta’s core team have been designing, supporting and delivering well-regarded behavioural interventions for 20 years. We can either deliver complete services or train and support local staff to deliver a licensed programme in teh heart of their communities. Examples of Momenta programmes include:
- Diabetes Prevention Programme (DPP): The only DPP selected for both NHS England’s national framework and use across all Northern Irish Health and Social Care Trusts
- Diabetes Remission Programme (DRP): We have been selected to deliver this programme as part of the NHS Type 2 Diabetes Path to Remission Programme national framework
- CVD Prevention Programme (CPP): Co-developed with the NHS, with input from the British Heart Foundation, Momenta’s 9-month CPP is currently being delivered to patients in a number of areas across the UK. Similar to Diabetes Prevention Programmes it is provided to patients over a 9-month period in 18 x one-hour sessions delivered by trained Coaches.
The Heart Health Check has been adapted from an existing intervention used in secondary care in Northern Ireland, which we were fortunate to co-develop with the South Eastern Health and Social Care Trust. It is based on research showing the success of similar brief interventions for smoking cessation, alcohol reduction and obesity management.
You can find out more about us at Discover Momenta.